The Benefits of Advanced DED Diagnostics
Provide your patients with minimally invasive options that offer fast results.
KEY TAKEAWAYS
- Advanced dry eye disease diagnostic devices are minimally invasive and provide fast data acquisition.
- Patient success is contingent on patient history, multimodal diagnostic testing, and monitoring treatment response.
- Patients can receive personalized treatments in both a comfortable and timely manner.
Advanced dry eye disease (DED) diagnostic devices are minimally invasive and provide fast data acquisition. Given these attributes, optometrists should consider implementing one or more of them in their practices. A caveat: Patient success is contingent on patient history, multimodal diagnostic testing, and monitoring treatment response.
Here, I discuss the latest advanced DED diagnostics in terms of their clinical utility.
OSMOLARITY SYSTEMS
These devices assess the tear film for an increase in osmolarity, or an above-normal level of salt in the tears. As an increase in osmolarity indicates a loss of homeostasis of the tear film, it is a criterion for diagnosing DED.1 Currently, one osmolarity device is FDA-cleared: the ScoutPro Osmolarity System (Bausch + Lomb).
Minimally Invasive
Tear osmolarity requires a small (nanoliter) sample from the lower lid tear meniscus (not the central cornea) with brief contact, all the while keeping the ocular surface intact. Additionally, no corneal dyes or topical anesthetics are required. Further, most patients report experiencing little to no discomfort.
Fast Data Acquisition
The ScoutPro provides data in about 15 seconds per eye from setup to lab result.
MEIBOGRAPHERS
Imaging of the meibomian glands aids in the diagnosis of meibomian gland dysfunction (MGD), the most common cause of evaporative DED (Figure). This is because these devices enable us to visualize meibomian gland structural changes, such as tortuosity, dilation, and truncation. Tortuosity of the lower eyelid is correlated with DED symptoms.1 Also, meibomian gland length is a key morphological metric in terms of gland expressibility, with shorter glands showing less expression.2 Meibographers that are FDA-cleared include the HD Analyzer (Keeler) and the LipiScan Dynamic Meibomian Imager (Johnson & Johnson).
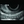
Minimally Invasive
Images of the meibomian glands are obtained via infrared transillumination through the lid with simple lid eversion.3 Additionally, no corneal dyes, topical anesthetics, or dilation is required. Patients typically report mild awkwardness in undergoing meibography, though no pain. Further, patients do not complain of blurred vision, irritation, or photophobia after the fact.
Fast Data Acquisition
Meibographers take about 1 to 3 minutes from patient setup to the acquisition of diagnostic images.
OCULAR SURFACE INTERFEROMETERS
These devices provide an objective measurement of the thickness of the tear film’s lipid layer. This is significant, as the tear film lipid layer’s thickness acts to prevent aqueous layer evaporation. These devices provide this objective measurement by identifying interference patterns in the lipid layer.1 These patterns correlate to corneal staining and tear breakup time (TBUT), thus aiding in the diagnosis of MGD.1 The FDA-cleared ocular surface interferometer is the LipiView II Ocular Surface Interferometer (Johnson & Johnson).
Minimally Invasive
These devices do not encounter the conjunctiva, cornea, or lids, as tear film thickness measurement is acquired via reflected light patterns. Further, no dyes or topical anesthetics are used. Patients focus on a target and are instructed to blink normally.
Fast Data Acquisition
From patient preparation and positioning to measurement per eye, the total time is roughly 1 to 5 minutes.
MATRIX METALLOPROTEINASE-9 (MMP-9) TESTING
MMP-9 is an inflammatory marker that is elevated in the tears of patients who have severe DED.1 According to the Tear Film & Ocular Surface Society Dry Eye Workshop III report, which was released in June 2025, MMP-9 is a second criteria that can be used to diagnose DED. This is because it also indicates a loss of homeostasis of the tear film.1 The InflammaDry (QuidelOrtho) is the FDA-cleared MMP-9 test.
Minimally Invasive
The InflammaDry briefly contacts the palpebral conjunctiva for a tear sample, so no ocular tissues are penetrated. Additionally, topical anesthetic is not required.
Fast Data Acquisition
Tear sample acquisition takes less than 1 minute, and results take roughly 10 minutes.
AI-ASSISTED DIAGNOSTIC DEVICES
Two DED diagnostic devices are available that are assisted by AI: the CSI Dry Eye Software (CSI Dry Eye Innovations) and the OmniCad Ocular Surface Imaging System (Quantel Medical/Lumibird Medical).
The CSI Dry Eye Software is a cloud-based platform that uses evidence- and AI-based algorithms.4 Additionally, the software provides treatment recommendations based on its findings and a patient education report to facilitate patient compliance to treatment.
The OmniCad Ocular Surface Imaging System measures blink rate, noninvasive TBUT, lipid layer thickness using interferometry, tear meniscus height, and meibography. Using this information, it then provides a disease severity assessment in an objective diagnostic report.5
COMBINATION DEVICES
Advanced DED diagnostic devices are also available in other combination systems. These systems can be comprised of ocular interferometry, meibography, blink dynamics, tear meniscus height, corneal topography, noninvasive TBUT, anterior segment photography, fluorescein imaging, pupillometry, conjunctival redness score, and wavefront aberrometry, to name some.5 These include the VX 120+ Dry Eye/Anterior Segment Analyzer (Visionix), the Keratograph 5M (Oculus), the Tera Dry Eye Imager (Topcon), and the Bruder Ocular Surface Analyzer (M&S).6-9
FORWARD-THINKING OUTLOOK
I believe these advanced DED diagnostic tests will make identifying DED faster, easier, and more efficient. This will, in turn, help make treatment more personalized and successful. We can prepare for the future now by remaining aware of all these diagnostic tools have to offer to better serve our DED patients.
PERSONALIZING TREATMENT
Based on the described attributes of the advanced DED diagnostic devices described, it’s clear they are useful additions to the diagnostic toolbox. To review, they enable patient comfort, while streamlining data acquisition. These benefits are a win-win for both DED patients and optometrists alike.
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!



